Today is Day 2 of Week 6 of the Covid-19 epidemic. Everyone is stressed. We are all dealing with our unique situations with a lot of commonality. Quarantining with family has its adventures, for sure. Fortunately, we have had only a handful of probable or clinically diagnosed Covid-19 infections among our members so far, but we have some substantial way to go.
Where are we, big picture? Lots of problems.
Total cases in Massachusetts continue to increase, now at 36,372 as of yesterday, with a new case count of 1970 as shown in Graph 1:
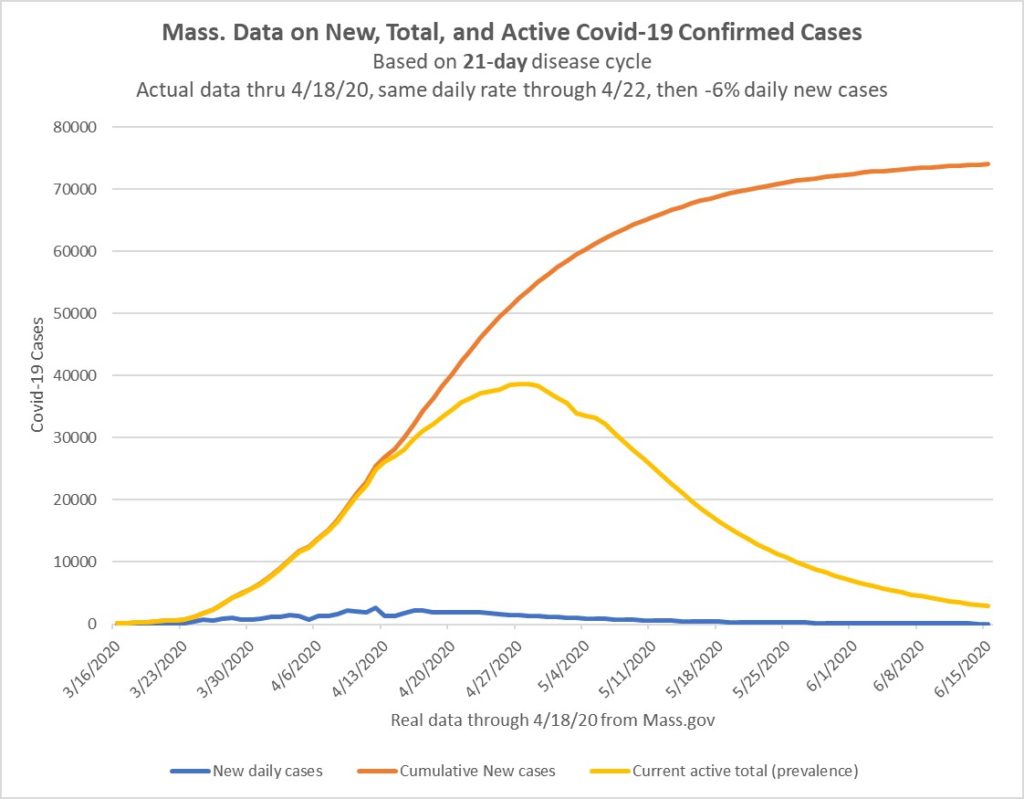
Graph 1: New case daily incidence, cumulative totals, and est. active disease prevalence. Actual case data to 4/18/20, projection afterward.
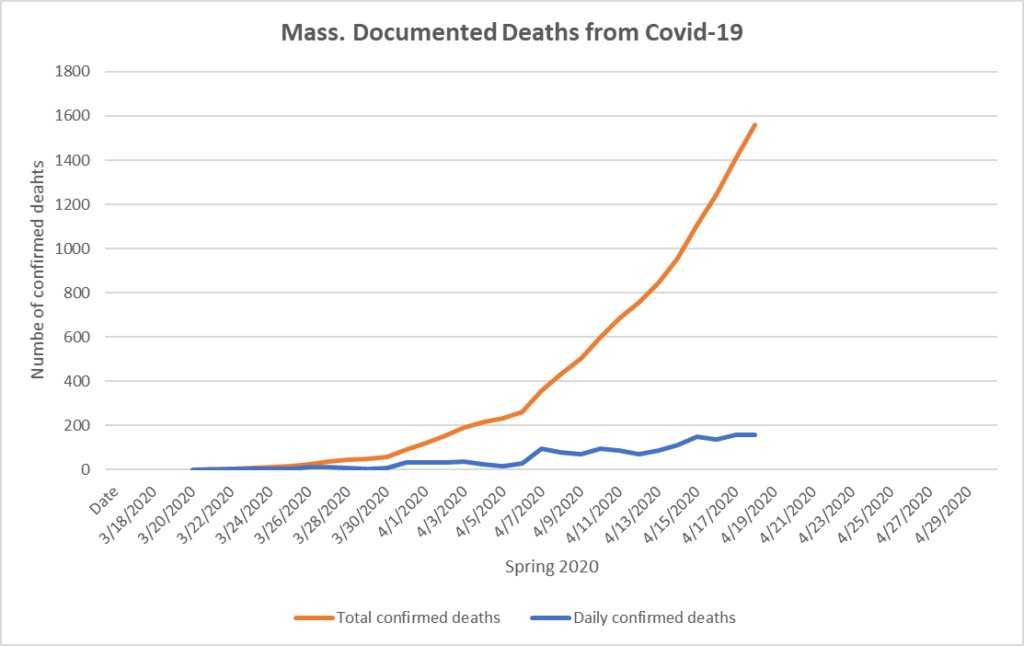
Daily confirmed Covid-19 deaths also have increased greatly, now total 1560, and were 156 yesterday as shown in Graph 2:
Hospitals remain under severe pressure. PPE (personal protective equipment) are progressively more available for hospital professionals, but it would be a big reach to say that medical professionals have what they need, or that individuals could readily find adequate masks or sanitizers. We are still behind and it is unclear when we will catch up.
Where are we? Perhaps some progress.
Testing is getting more available, so that ill patients can be screened with PCR tests in hospital settings, but more common ambulatory cases (of the sort we see among our members) still face enormous logistical difficulties to get the PCR test to confirm a clinical suspicion or personal worry.
However worrisome the two preceding graphs, there are public hard data from DPH that do seem to show that the rate of increase of daily confirmed new cases has lessened and appears to be flat for the past 5-7 days. This presumably would be the good result of the social distancing and work-place and school closures that have taken place.
A plateau would at least relieve some of the pressure on hospitals, but we really need a daily reduction in the number of new cases in order for real improvement to begin. A plateau at the current high level would still be difficult to manage.
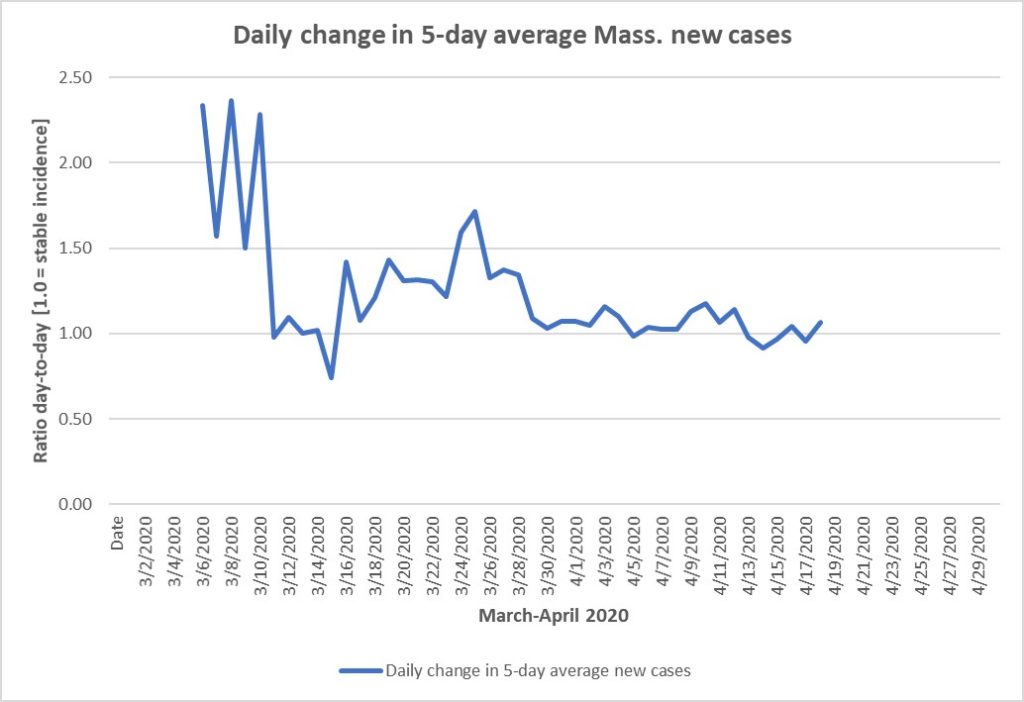
The next graph demonstrates the rate of change in the number of new cases each day. I have not seen this data presented this way elsewhere. The data for each day is in fact a 5-day average from the preceding 5 days to smooth the graph for legibility. The ratio is the the number of new cases (5-day average) on a day compared to day previous. Hence a value of 1.0 means the new cases are about the same, a value greater than 1.0 means new cases are increasing in number each day, while a value less than 1.0 means new cases are diminishing (though clearly still present):
It is apparent that in early March the number of new cases was increasing by a factor of 1.5 to 2.0 (50% or 100% increase each day), while in the past week the new case ratio is hovering about 1.0, sometimes a bit lower, indicating that the daily number of new cases in not increasing and may be beginning to decrease. This is great news and going on long enough to hope that this trend will hold up and perhaps truly head downward.
What do we do for now?
We continue to shelter in place and work from home as much as possible. That is an effective strategy for safety. We wash our hands frequently (never have so many people sung Happy Birthday so frequently!). We go to stores infrequently if we can manage that. We wear face masks that we purchase or make up when we are out. They help for ordinary public interactions, along with clear distancing. How much the non-N95 masks help protect the wearer as opposed to others remains under argument, but in conjunction with rigorous physical distancing a mask should be incremental benefit. (Clearly we will all happily buy manufactured new masks, a good surgical variety or preferably N95, when production eventually catches up.)
We can worry less about the mail and packages and food. Those are really low down on the infection risk list. The New York Times just had an excellent article yesterday with experts commenting reassuringly on these issues.
We do have to figure out how to get together socially without being together to maintain family and friend relationships. We do need new ways to attend to our own bodies, eating properly under stress and trying to get in some exercise without going to a gym. And how to get one’s hair done! Who knew? (I am now 6 weeks post haircut and doing the full Bernie at the moment. My wife Linda, who used to cut my hair, may come to the rescue soon.)
But we do need to stay psychologically prepared for this semi-quarantine, restricted-public-access life for at least another month. Even with better results on daily new infections, the prevalence of Covid-19 in the community will remain high (based on current figures) at least through May. Just review the prevalence numbers in the initial graph.
Why is Covid-19 so worrisome to all of us?
I know many of you are highly concerned about your own safety and general well-being, as well as that of your loved-ones. Dr. Sobel and I share your concerns. I also realize that I (and Dr. Sobel) both worry more about Covid-19 than any other infectious disease we have encountered. We have lived and worked through AIDS and hepatitis C, and the swine flu and other serious communicable diseases. We all know that this is different. Why?
First, Covid-19 morbidity and mortality figures are much worse than than annual influenza or pneumonias or any of the diseases I mentioned just above. The CDC data on their website are eye-opening. As of today, the total US cases are 690,714. Total deaths are 35,443. That’s a 5.1% death rate. The final mortality rate will be different, perhaps lower (if we get an effective treatment soon, or if there are a much larger number of mild and undetected or reported cases), or perhaps higher (if we do better enumeration of deaths that likely involved Covid-19 but where the infection wasn’t confirmed). Regardless, the annual death rate from influenza is on the order of 0.1% to 0.2% by comparison. [Yes, there are many fine points, such as which people with preexisting conditions, or age, or environment like a nursing home are more likely to die, but the risk for everyman or everywoman is high.]
Second, large proportions of people of all ages (though especially older people) end up in the hospital and the ICU. That is simply not the case with other common infectious diseases. CDC numbers for the US just cited indicate 19% of all patients with documented Covid-19 require hospitalization, and 1/3 of them (about 6%) end up in the ICU. That remains staggering to conceive of.
Third, we have no known curative therapy at this time. We have drugs under investigation, drugs under development, possibly immune globulin infusions and so forth. But even the most enthusiastic (realistic) reports about specific treatments talk of modest or incomplete results. And we’d still have to ramp up production and distribution of any new successful drug in light speed. The epidemic is peaking now.
Fourth, while PCR tests are becoming more available, there are concerns about reported high false negative rates of the PCR tests in the field, and regardless we do not yet have true capacity to test all ill people. Nor do we now have high capacity to do serum antibody testing (for IgG and IgM) to determine if someone has had the Covid-19 virus and has protective antibodies. In fact, one of our members runs a biotech company developing a simple fingerstick antibody test for Covid-19. They will be looking for volunteers with documented Covid-19 (or highly likely infection clinically) to standardize their new test. This will not be for official clinical testing. I will circulate the details when confirmed later next week.
Fifth, because Covid-19 is highly contagious, and because we have learned that many people with the disease are asymptomatic, and because CDC and others now affirm that there is some infectivity of Covid-19 in people who are presymptomatic or asymptomatic with the infection, how does anyone determine who is a safe person to be with in close quarters? We will not know that until there is widespread antibody testing not only available but actually administered. That’s some time away.
How to emerge from self-quarantine
We are not leaving quarantine anytime soon, but it may help clear our minds and lighten our hearts to think about that time. The question of the requisites to start to resume normal life becomes fairly straightforward based on the above. I hope this short discussion provides useful context when you hear others talk about or read about any “plan” to return to normal or to “open” the country.
First, we need an effective, readily available treatment for Covid-19 so that an exposure and infection doesn’t mean a 20% likelihood of hospitalization with a 6% chance of needing an ICU and a 5% overall chance of death (again, in the aggregate).
Second, we need a readily available serum antibody test (home testing by fingerstick comes to mind, or saliva) for everyone to learn if they do or do not have antibody to Covid, and if it is protective (we still are not sure, by the way, that presence of antibody necessarily confers immunity). And to be able to determine the status of people you might interact with.
Third, we need readily available secure personal protective equipment, specifically N95 masks or equivalent, together with adequate hand sanitizer and wipes (you can’t always get to a sink), so that being in close quarters with another human is less risky or at least of known risk. We shouldn’t have to settle for less secure PPE not because they wouldn’t provide additional benefit, but because they are not available!
Fourth, we eventually need an effective vaccine against SARS-CoV-2 (the causative virus for Covid-19) that is proven, safe and pervasively available. There seems to be little likelihood of such a vaccine ever being deployed fully until well into 2021, if not later. But we can hope for results promising for effectiveness sometime this year.
Final thoughts
This is a unique event in our history. For now we need to continue to pay careful attention to our safety and that of family and friends. We can be hopeful in Massachusetts (which is worse than much of the country) that daily new cases will start to drop and eventually the prevalence of the infection will be substantially reduced by end of May or sometime in June. We should begin to focus on what information you would want to venture out of your circle of safety? How could we go to a restaurant again? What would make you feel safe? Or to go to a hairdresser? Same issue. Your opinions matter. Your personal risk/benefit calculus matters.
We will continue to send you updates weekly or possibly more often on the epidemic. Dr. Sobel and I will also continue to do remote office visits at least through the end of this month and likely for well into May. They seem to be effective, perhaps more than we thought. Nevertheless, we sincerely look forward to resuming office visits when we can do so with safety for you and us.


Thank you for the updates, Dr. Kanner. The straightforward, detailed information is very helpful. My family and friends truly appreciate them.
Thank you. Questions are welcome. And friends can sign up themselves on the various SignIn links on the blog pages.
really great updates. Thanks
I very much appreciate these updates. Thank you!
Reopening the country without appropriate protective gear and strategies will endanger lives more than is necessary. For those who choose this, such as the Michigan protesters, it is their risk decision to make, although it will also recklessly endanger others. For those who don’t choose this, such as the nation’s medical workers, it is exploitive and unfair to expect them to put their lives on the line without appropriate protection. The government will be sending them to their execution. Medical workers should stay home for their own safety unless the government can provide them the protection science says they need and what they deserve. With such protection, some may still get sick, but at least we will know we’ve done the best we can while we remain deeply grateful for their service.
The correct reopening logic is simple: reopen with appropriate protection or reopen irresponsibly without protection but also without a medical mop-up force.
“Appropriate protection” includes a sufficient supply of PPE so medical workers can follow the safety protocols they were taught along with available/actual testing sufficient to allow contact tracing with enforceable quarantine requirements of positive cases, including asymtomatics.
One might argue that a medical worker strike is contrary to the Hippocratic Oath. Ethicists must ask if deliberate endangerment due to purely political and financial interest with knowledgeable disregard for health safety requirements justifies such action. Undoubtedly there will be medical individuals willing to sacrifice themselves to help others under any circumstances, but are we as a society willing to say it should be institutionalized when there is a safer alternative?
I appreciate your thoughtful reflections on a very real and difficult situation. I would perhaps say that the government “may be” rather than “will be” sending the medical workers to their deaths as more proportionate description, but the point is well taken. Thanks for engaging this thorny issue.
This is the best graph I have seen about where we are with this virus:
https://aatishb.com/covidtrends/
Here is a video that explains the graph:
https://youtu.be/54XLXg4fYsc
Thanks. I think it is a useful display of multi-country data.
There is a lot of very recent talk about the role of blood, and the possibility of blood clots. Epitomized by the amputation of the Broadway actor’s leg. Is there anything that folks who take blood thinner (like me)should ponder about this?
I believe the issue is hypercoagulability induced by the Covid-19 infection that produces intravascular coagulation. Anticoagulation of the sort you are on should be protective. But that gets difficult to monitor during severe illness. So this will ultimately be an inhospital ICU sort of issue to deal with, not something that has any operational import if you are at home and securely staying out of circulation, as you are.